Medical Oxygen Supplies at Home: What You Need and Where to Get It
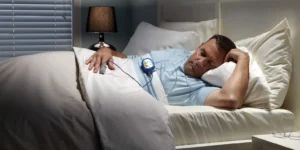
Apr 07 2026 Home Oxygen MachineThis guide explains the core medical oxygen supplies for home use, what to ask for, and where people usually get them in the UK.
Who typically needs medical oxygen at home?
People usually need home oxygen when a clinician confirms low blood oxygen levels and prescribes oxygen therapy. Common reasons include COPD, pulmonary fibrosis, severe asthma, bronchiectasis, pulmonary hypertension, some heart conditions, and recovery after serious respiratory illness.
They should not self-prescribe oxygen. The correct flow rate, hours per day, and delivery method are clinical decisions, and the wrong setup can cause harm or delay proper treatment.
What types of home oxygen systems are available?
Most home set-ups fall into three categories: oxygen concentrators, oxygen cylinders, and liquid oxygen systems. The best choice depends on prescription, mobility needs, flow rate, and how many hours per day they require oxygen.
Many people have more than one system. For example, a stationary concentrator for daily use at home plus a small cylinder for backup during power cuts or for short trips.
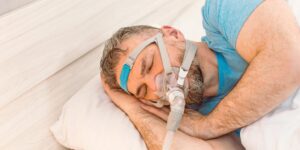
What is an oxygen concentrator, and when is it used?
A concentrator is usually the main home oxygen device because it makes oxygen from room air. It plugs into the mains and delivers a prescribed flow through tubing to a nasal cannula or mask.
Concentrators suit people who need oxygen for long periods each day. They reduce reliance on deliveries, but they need electricity, good ventilation, and basic upkeep such as cleaning filters as instructed by the supplier.
When are oxygen cylinders necessary?
Cylinders are often used for portability or as backup if electricity fails. They store compressed oxygen and deliver it through a regulator that controls the flow rate.
They are useful for short outings, emergencies, or for people who only need oxygen intermittently. However, cylinders run out, must be stored safely upright and secured, and require planning so replacements arrive before they are empty.
What is liquid oxygen, and who is it for?
Liquid oxygen systems store oxygen in a cooled liquid form and can provide higher flow rates and longer portable use than many small cylinders. They are typically offered to people with higher oxygen demands or those who need longer periods away from home.
Not everyone is eligible, and availability can vary by region and clinical criteria. The supplier normally provides the storage vessel and portable units, plus training for safe refilling and handling.
What accessories and consumables do people usually need?
Most people need a delivery interface and basic consumables that keep therapy comfortable and hygienic. Typical items include nasal cannulas, oxygen masks (if prescribed), oxygen tubing, connectors, and sometimes a humidifier bottle if dryness is an issue and it is approved for their set-up.
They may also need skin-friendly tape, spare cannulas, and a simple storage solution to prevent tubing becoming a trip hazard. They should only use parts compatible with their prescribed equipment.
What safety equipment and home adjustments are essential?
Oxygen increases fire risk, so safety supplies and habits matter as much as the device. At a minimum, they should have visible “Oxygen in use” signage, keep equipment away from flames and heat sources, and follow strict no-smoking rules inside the home.
They should also reduce trip risks by routing tubing carefully, avoiding oil-based creams near the face, and keeping cylinders secured. If they use a concentrator, they may need a backup plan for power cuts agreed with their oxygen provider.
Where do people get home oxygen in the UK?
In the UK, home oxygen is usually provided through the NHS after specialist assessment and a prescription. A clinical team arranges the order, and an authorised home oxygen supplier delivers, installs, and provides patient training.
Private purchase exists, but it is rarely the best first step for long-term therapy. If they believe they need oxygen, they should start with their GP or respiratory team so the underlying cause is assessed and the correct prescription is set.
What is the difference between NHS-provided oxygen and buying privately?
NHS oxygen is prescribed, delivered, and supported, which usually includes maintenance and replacement parts under the service arrangement. It is designed for medical use with clinical oversight and a clear escalation pathway if needs change.
Private options can be expensive and may still require a prescription depending on the supplier and intended use. If they buy privately without proper assessment, they risk using the wrong flow rate, missing a serious diagnosis, or relying on equipment without adequate servicing.
What should they ask a supplier or clinician before oxygen is delivered?
They should confirm the prescribed flow rate, how many hours per day oxygen is needed, and whether it is for rest, sleep, exertion, or all three. They should also ask which device type is being provided and whether a backup cylinder is included.
Practical questions matter too: delivery times, emergency contact details, servicing schedule, consumable replacement process, and clear training on alarms, cleaning, and safe storage. If they travel, they should ask how portability and holiday cover work.
How can they prepare the home before installation?
They should choose a well-ventilated space for the main device, near a safe power source, and with enough room to avoid blocking vents. If they use long tubing runs, they should plan a route that reduces tripping and avoids doorways where tubing can snag.
They should also set household rules early, especially no smoking indoors, and keep candles, gas hobs, and heaters at a safe distance. A quick checklist on the fridge can help everyone follow the same safety steps.
What are the most common mistakes with home oxygen supplies?
The most common mistake is treating oxygen like a general “breathing booster” rather than a prescribed medicine. People also underestimate fire risk, store cylinders poorly, or use the wrong accessories because they seem interchangeable.
Another frequent issue is running out of portable oxygen during outings due to poor planning. They should learn their device’s run time, keep spares where appropriate, and contact the provider early if symptoms change or oxygen needs increase. For additional support, explore breathing exercises that can help improve lung function and breath control.
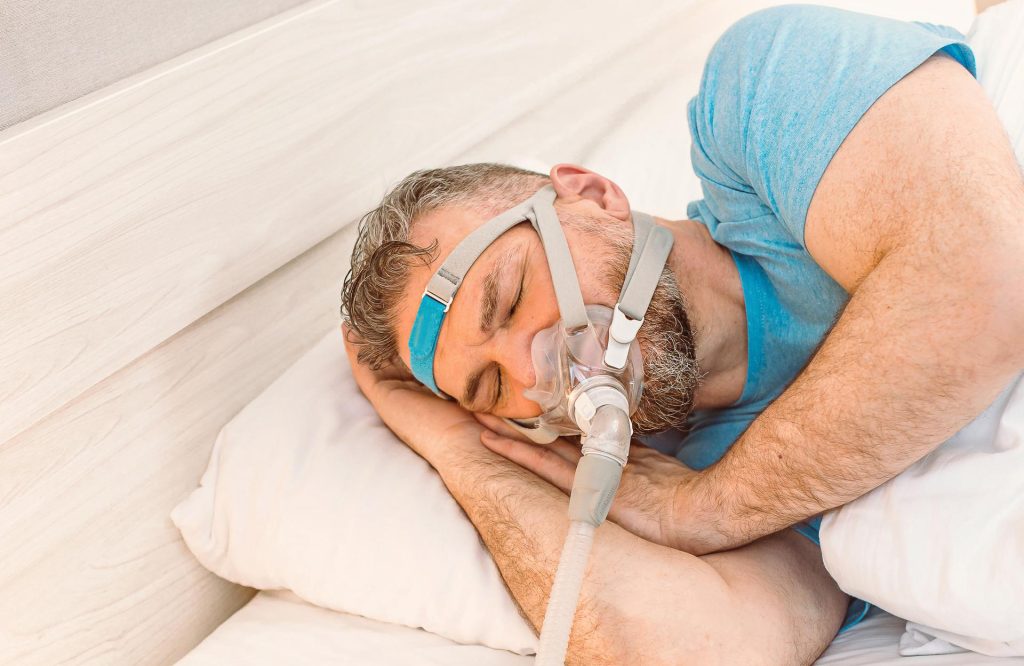
Where can they get urgent help if something goes wrong?
If equipment fails, they should contact the home oxygen supplier’s emergency number, which is provided during installation. For worsening breathlessness, chest pain, blue lips, confusion, or collapse, they should treat it as a medical emergency and seek urgent care.
They should never adjust flow rates beyond the prescription unless a clinician instructs them to. If they feel their current prescription is no longer enough, they should request a clinical review rather than trying to “turn it up” themselves.
What is a simple checklist of what they need at home?
They usually need the oxygen source (concentrator, cylinders, or liquid oxygen), the right interface (nasal cannula or mask), tubing and connectors, and a safe storage plan. They should also have written safety rules, supplier contact details, and clear instructions for cleaning and replacing consumables.
Most importantly, they need a confirmed prescription and follow-up plan. Home oxygen works best when equipment, training, and clinical review are treated as one complete package.
More to Read : What Is an OPEP Device? How the Aerobika Helps Clear Mucus
FAQs (Frequently Asked Questions)
Who typically needs medical oxygen therapy at home?
Home oxygen therapy is usually prescribed for people diagnosed with low blood oxygen levels by a clinician. Common conditions include COPD, pulmonary fibrosis, severe asthma, bronchiectasis, pulmonary hypertension, certain heart conditions, and recovery after serious respiratory illnesses. Oxygen should never be self-prescribed as the correct flow rate and delivery method require clinical assessment.
What types of home oxygen systems are available in the UK?
The main types of home oxygen systems include oxygen concentrators, oxygen cylinders, and liquid oxygen systems. The best option depends on individual prescription needs, mobility requirements, flow rates, and daily usage hours. Many patients use a combination, such as a stationary concentrator at home and portable cylinders for outings or backup.
How does an oxygen concentrator work and who is it suitable for?
An oxygen concentrator extracts oxygen from room air and delivers it through tubing to a nasal cannula or mask. It requires mains electricity and good ventilation. Concentrators are ideal for individuals needing long periods of oxygen daily as they reduce reliance on deliveries but require regular maintenance like filter cleaning according to supplier instructions.
When are oxygen cylinders necessary for home use?
Oxygen cylinders store compressed oxygen and are often used for portability during short trips or as backup during power outages. They deliver oxygen via a regulator controlling flow rate but need careful storage upright and secured. Cylinders run out and require timely replacement planning to ensure continuous supply.
What safety measures should be taken when using medical oxygen at home?
Oxygen increases fire risk; therefore, safety is paramount. Essential precautions include displaying ‘Oxygen in use’ signs visibly, keeping equipment away from flames and heat sources, enforcing strict no-smoking rules indoors, securing cylinders properly, managing tubing to prevent tripping hazards, avoiding oil-based creams near the face, and having a power cut backup plan if using concentrators.
How can patients in the UK obtain home oxygen supplies safely?
In the UK, home oxygen is typically provided via the NHS following specialist assessment and prescription. A clinical team arranges delivery through authorised suppliers who install equipment and provide training. While private purchase options exist, starting with a GP or respiratory specialist ensures proper diagnosis and prescription to avoid risks associated with incorrect usage or equipment.