Why a CPAP Sleep Study Can Fast-Track Your Treatment Plan
Mar 20 2026 UncategorizedWhat is a CPAP sleep study, and how is it different from a regular sleep study?
A CPAP sleep study is a monitored night of sleep where clinicians evaluate breathing and, if needed, start CPAP therapy during the study. Unlike a diagnostic-only study that simply confirms sleep apnea, a CPAP-focused study also tests treatment in real time.
In many labs, this is done as part of a CPAP sleep study, often conducted as a “split-night” study where the first part diagnoses the condition and the second part titrates CPAP settings once apnea is clearly seen.
How does a CPAP sleep study confirm whether they actually need treatment?
It identifies how often breathing events happen, how severe they are, and how much oxygen drops during sleep. That matters because symptoms alone can be misleading, and severity helps determine urgency and the best treatment path.
The study also shows patterns, like whether events worsen in REM sleep or when they sleep on their back, which can influence therapy decisions and expectations.
Why can it shorten the time from diagnosis to feeling better?
It reduces guesswork. Instead of diagnosing apnea and then scheduling a second appointment or trial period to adjust therapy later, a CPAP sleep study can move directly into choosing a workable pressure range and setup.
When they leave with a clearer prescription and a more confident plan, they often spend less time cycling through discomfort, ineffective settings, or repeated follow-ups just to reach stability.
What does “titration” actually do for their CPAP prescription?
Titration finds the pressure needed to keep the airway open across different sleep stages and positions. The goal is not just “some pressure,” but the lowest effective pressure that reliably prevents events and improves oxygen levels.
That precision can help them avoid common early problems, like persistent snoring on CPAP, waking up gasping, aerophagia from overly high pressure, or a lingering sense that therapy “isn’t working.”
How does it help choose the right mask and comfort settings?
A study can reveal issues that are hard to spot at home, such as mouth breathing, leak patterns, or discomfort that causes frequent awakenings. Technicians can swap masks, adjust fit, or add comfort settings on the spot.
That early troubleshooting can be the difference between someone who tolerates CPAP from week one and someone who abandons it after a few frustrating nights.
Can a CPAP sleep study prevent weeks of trial-and-error with an at-home setup?
For many people, yes. Home trials can work well, but they rely on gradual adjustments and user feedback, and some problems only show up clearly under monitoring.
A CPAP sleep study can quickly answer questions like whether pressure needs to vary during the night, whether they need bilevel support, or whether leaks are undermining therapy, so they are not stuck “testing” indefinitely.
When is a split-night CPAP study especially useful?
It is often useful when moderate to severe sleep apnea is suspected and there is a high likelihood they will need CPAP. In those cases, a split-night approach can compress diagnosis and treatment into one appointment.
It can also help when symptoms are disruptive and time matters, such as severe daytime sleepiness, safety-sensitive jobs, or significant oxygen drops that suggest they should not wait months to optimize therapy.
What should they expect during the night?
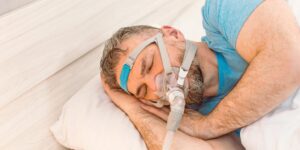
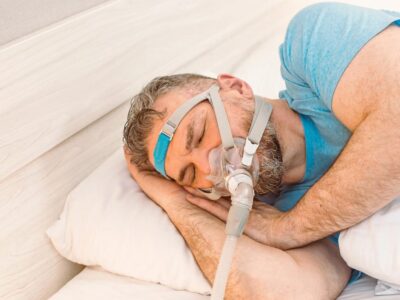
They will sleep with sensors that monitor breathing, oxygen, heart rate, sleep stages, and movement. If CPAP is introduced, they will wear a mask connected to a machine while staff adjust settings to reduce breathing events.
It can feel unfamiliar at first, but the lab environment is designed for this, and the staff can respond immediately if they feel claustrophobic, overly pressured, or unable to settle.
What happens after the study, and how does it speed up the next steps?
The results typically produce a clear treatment recommendation and a prescription that includes pressure settings and therapy type. With a stronger starting point, their equipment provider and clinician can move faster and make fewer changes later.
They should still expect some fine-tuning in the first weeks, but the baseline is usually closer to what they actually need, which can speed up comfort and symptom improvement. Learn more about bulk-bill sleep study Perth: availability, wait times, and tips.
How can they get the most value from a CPAP sleep study?
They should share relevant details upfront, including usual sleep position, nasal congestion, prior mask concerns, and any anxiety about CPAP. Bringing their typical bedtime routine, avoiding heavy alcohol before the test, and asking how results will be communicated can also help.
Most importantly, they should treat the study as the start of a plan, not a one-night verdict. The faster the first setup is right, the faster they can feel like themselves again.
FAQs (Frequently Asked Questions)
What is a CPAP sleep study and how does it differ from a regular sleep study?
A CPAP sleep study is a monitored night of sleep where clinicians not only diagnose sleep apnea but also initiate and adjust CPAP therapy during the same study. Unlike a regular diagnostic-only sleep study that simply confirms the presence of sleep apnea, a CPAP-focused study tests treatment in real time, often using a split-night approach where the first part diagnoses and the second part titrates CPAP settings.
How does a CPAP sleep study confirm if treatment is necessary?
The study measures how often breathing disruptions occur, their severity, and oxygen level drops during sleep. These objective data points help determine the urgency and best treatment path, as symptoms alone can be misleading. It also identifies patterns like worsening events during REM sleep or when sleeping on the back, influencing therapy decisions.
Why can a CPAP sleep study shorten the time from diagnosis to symptom relief?
By combining diagnosis and treatment titration into one session, it eliminates the guesswork and delays associated with separate appointments or trial periods. Patients leave with clearer pressure settings and mask choices, reducing time spent on ineffective therapy adjustments or repeated follow-ups, thus speeding up comfort and symptom improvement.
What role does titration play in determining my CPAP prescription?
Titration identifies the lowest effective pressure needed to keep your airway open across different sleep stages and positions. This precision helps prevent common early issues like persistent snoring, waking gasps, discomfort from high pressure, or feelings that therapy isn’t working by ensuring optimal pressure tailored to your needs.
How does a CPAP sleep study help select the right mask and comfort settings?
During the study, technicians observe factors like mouth breathing, air leaks, or discomfort causing awakenings. They can immediately try different masks, adjust fit, or add comfort features to find what works best for you. Early troubleshooting increases tolerance to CPAP therapy from the start and reduces frustration that might lead to abandonment.
Can a CPAP sleep study reduce weeks of trial-and-error compared to at-home setups?
Yes. While home trials rely on gradual adjustments and user feedback, some problems only become clear under clinical monitoring. A CPAP sleep study quickly determines if pressure needs vary during the night, if bilevel support is necessary, or if leaks are compromising therapy effectiveness—helping avoid prolonged testing periods at home.
Read More